Advantages of tattoo-free deep inspiration breath hold
Postoperative radiotherapy after breast conserving surgery is standard of care for most patients. As well as improving rates of locoregional control, radiotherapy reduces the risk of breast cancer-related mortality compared with patients receiving surgery alone.1,2
However, breast radiotherapy is not without the potential for iatrogenic adverse effects or complications.1,2
Deep inspiration breath hold (DIBH) was introduced as a strategy to minimise irradiation to organs proximal to the breast.1,2
In addition, patient positioning methods during DIBH radiotherapy allows clinicians to depart from the historical permanent tattoo markings to tattoo-free systems, reducing the emotional burden on cancer survivors.3
GenesisCare has been at the forefront of introducing the routine use of DIBH for all left-sided breast cancer patients and are the first independent oncology provider in the UK to formally implement DIBH for right-sided breast cancers, as standard.
The deep inspiration breath hold technique
DIBH is well-established and beneficial during breast cancer treatment, particularly in terms of the reduction in cardiac morbidity.1,2
Clinical data is limited as cardiac toxicity from irradiation is subject to a protracted latency period. However, comparisons of heart dose parameter data suggest that DIBH can significantly improve both mean heart and left descending artery (LAD) doses, with studies indicating the mean heart dose may be reduced by up to 67% and mean LAD dose by up to 73%.2
As the relative risk of ischaemic heart disease may be decreased by 7.4% for each 1 Gy decrease in mean heart dose,7 this is of considerable clinical significance.
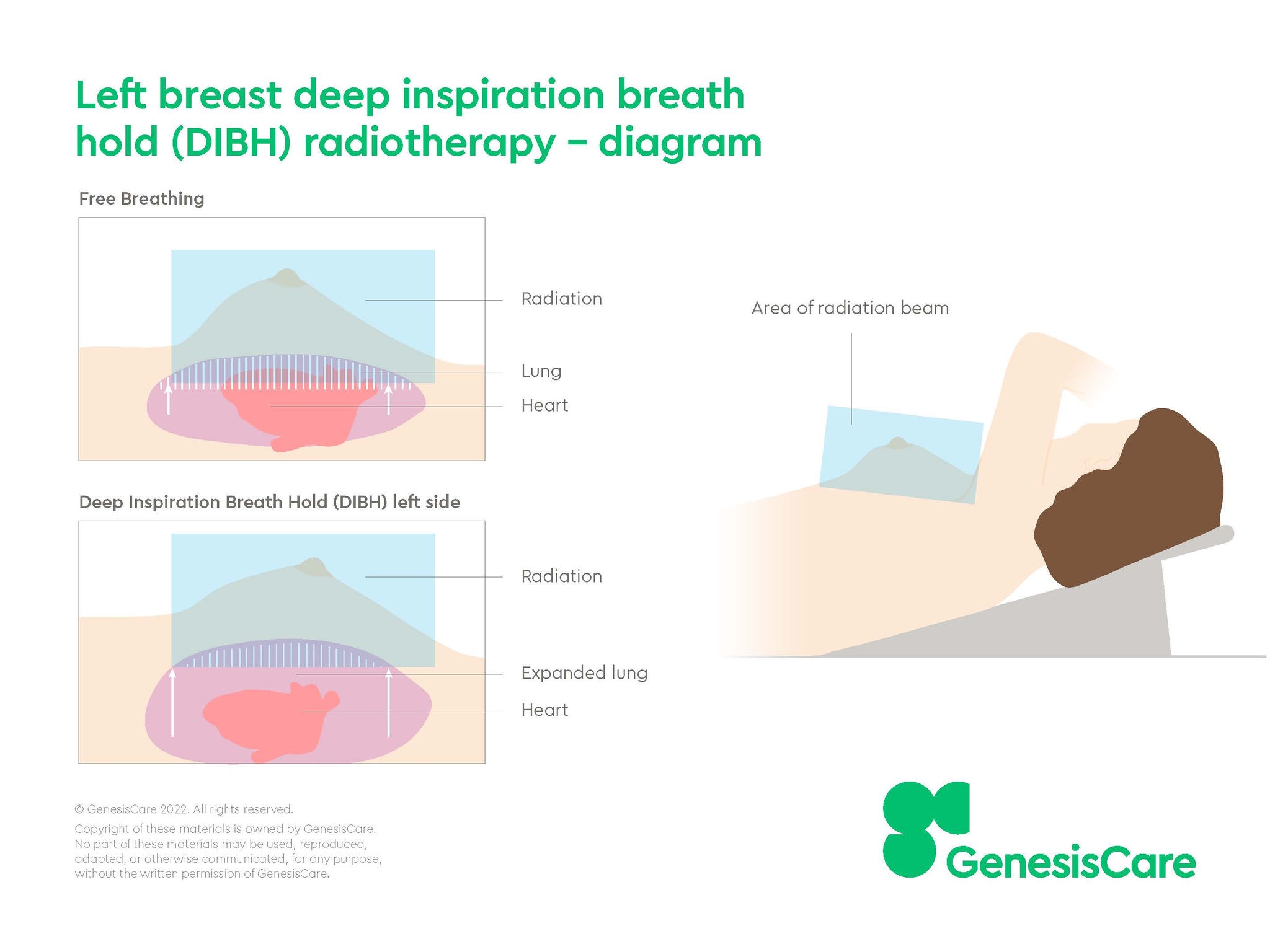
The premise of DIBH in aiding cardiac sparing during radiotherapy is based on the observation that during inspiration flattening of the diaphragm and inflation of the lungs moves the heart away from the chest wall.2
Left-sided DIBH
Right-sided DIBH
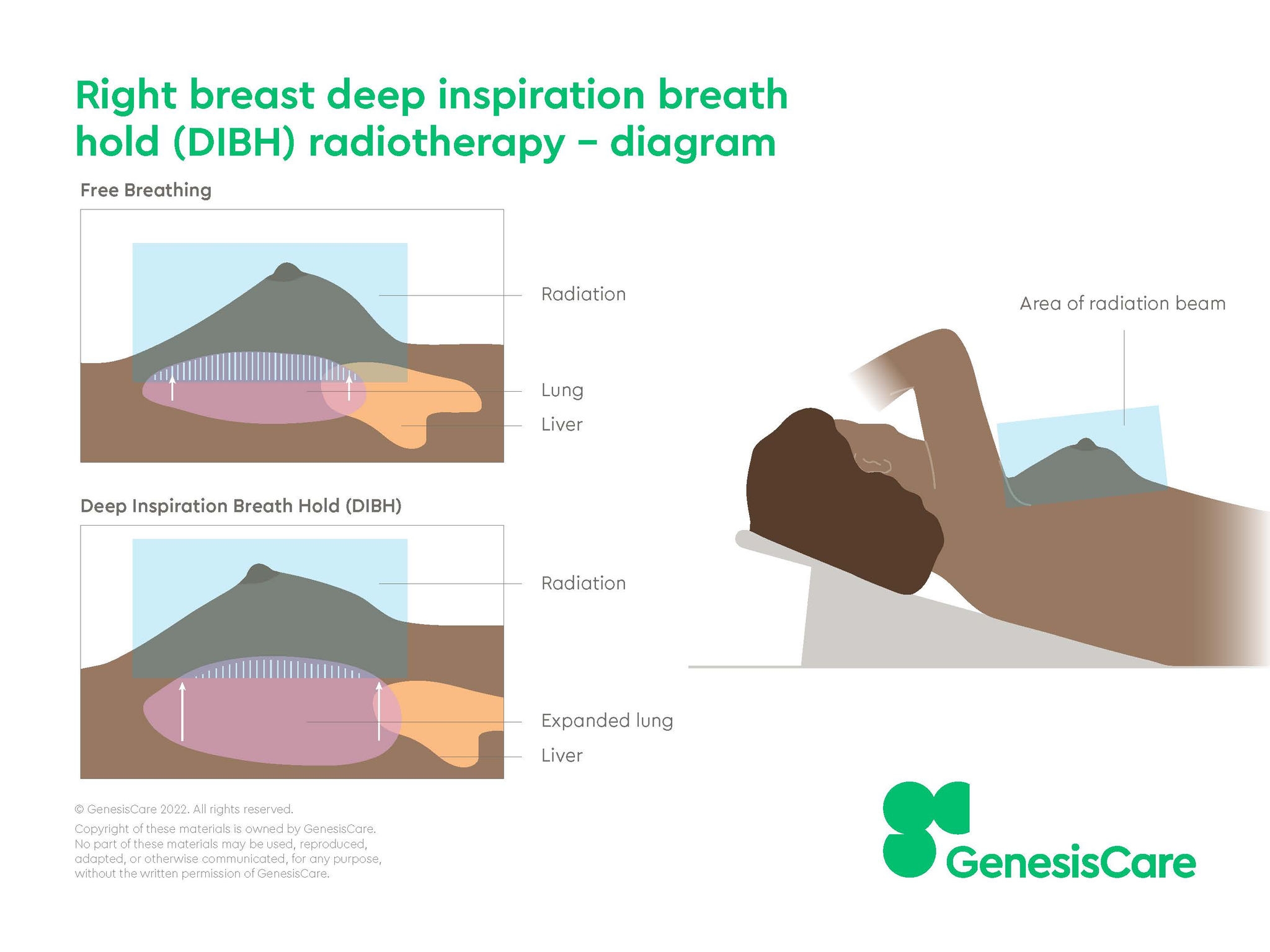
Find out more about DIBH and how it can help your patient during radiotherapy.
While the cardiac benefit of left sided DIBH is significant, DIBH may still be useful for patients receiving treatment to the right breast as the technique reduces lung exposure during irradiation of the internal mammary chain.2
During DIBH, patient positioning and alignment may be achieved using various tools. These include:
- Permanent subcutaneous tattoo markings
- Optical tracking systems
- Magnetic sensors2
As tattoo markings are associated with a significant psychological impact on breast cancer survivors,3 there is now a meaningful movement amongst clinical providers towards tattoo-free options.
At GenesisCare we use specialist motion and breath-hold techniques to protect the heart and lungs during radiotherapy, without the need for permanent tattoos or skin markings.
The psychosocial impact of tattoos on breast cancer survivors
During a period where breast cancer patients often report feeling vulnerable, disempowered, and dehumanised,4 permanent tattoo markings as part of the course of radiotherapy can add a further emotional burden.3,4
Investigations into the impact of tattoo markings on breast cancer patients undergoing radiotherapy found that 70% viewed these involuntary body modifications negatively, while 78% would opt for a tattoo-free treatment if given the choice.5
Furthermore, body image scores have been reported to be higher in patients not subject to permanent markings during their treatment.5
One publication reported that women felt that “tattoos [compounded] the trials of dealing with significant physical changes to their breasts and bodies arising from diagnosis and treatment”, with the markings acting as a permanent reminder of their battle with cancer.6
In addition to detrimental effects on emotional well-being in cancer survivorship, tattoo markings have limitations in accuracy as they are placed on a surface that is elastic and subject to organic changes, particularly over the course of radiation.6
Instead, systems that rely on verifying patient position by imaging the entire skin’s surface, such as surface-guided radiotherapy (SGRT), may be used to successfully and accurately position the patient as well as monitor and compensate for patient movement.3,6
As tattoo-free patient positioning in radiotherapy becomes increasingly accepted, clinical providers should remain cognisant of the impact that treatment itself can have on breast cancer patients, not just the initial disease diagnosis. Strategies to minimise emotional and psychosocial trauma during radiotherapy without compromising clinical safety and efficacy are available and should be utilised appropriately.
That's why alongside tattoo-free radiotherapy, through GenesisCare's unique partnership with Penny Brohn UK, all patients with breast cancer have access to wellbeing support.
Based on research into the connections between psycho, neuro and immunology, Penny Brohn UK has designed a holistic approach to address the needs of people diagnosed with this life-changing disease that is proven to improve outcomes.
Find out more about DIBH at GenesisCare and how your patients can benefit from tattoo-free treatment.
References
- Latty D, Stuart KE, Wang W, Ahern V. Review of Deep Inspiration breath‐hold techniques for the treatment of breast cancer. Journal of Medical Radiation Sciences. 2015;62(1):74–81.
- Bergom C, Currey A, Desai N, Tai A, Strauss JB. Deep inspiration breath hold: Techniques and advantages for cardiac sparing during breast cancer irradiation. Frontiers in Oncology. 2018;8.
- Freislederer P, Kügele M, Öllers M, Swinnen A, Sauer T-O, Bert C, et al. Recent advances in surface guided radiation therapy. Radiation Oncology. 2020;15(1).
- Probst H, Rosbottom K, Crank H, Stanton A, Reed H. The patient experience of radiotherapy for breast cancer: A qualitative investigation as part of the support 4 all study. Radiography. 2021;27(2):352–9.
- Breast Journal publishes impact of tattoos on radiation therapy patients [Internet]. Vision RT. 2022 [cited 2022 Dec 6]. Available from: https://www.visionrt.com/the-breast-journal-publishes-impact-of-tattoos-on-radiation-therapy-patients/
- Stanley DN, McConnell KA, Kirby N, Gutiérrez AN, Papanikolaou N, Rasmussen K. Comparison of initial patient setup accuracy between surface imaging and three point localization: A retrospective analysis. Journal of Applied Clinical Medical Physics. 2017;18(6):58–61.
- Simonetto C, Eidemüller M, Gaasch A, Pazos M, Schönecker S, Reitz D, et al. Does deep inspiration breath-hold prolong life? individual risk estimates of ischaemic heart disease after breast cancer radiotherapy. Radiotherapy and Oncology. 2019;131:202–7.

