Our approach is guided by a structured framework that supports ongoing review, evaluation, and continuous improvement.
Our quality program is aligned to the National Model for Clinical Governance and focuses on four priority areas:
- Safe - We actively manage and improve safety and quality systems to reduce risk and protect patients.
- Well-led - Strong governance and leadership drive accountability and continuous improvement.
- Caring and responsive - We work in partnership with patients, carers, and clinical teams to deliver care that meets individual needs.
- Effective - We monitor performance to ensure care is safe, high quality, and delivered efficiently by experienced clinical teams.

We collect and analyse data to understand how well we are delivering care and where we can improve. This is done in line with our Privacy Policy.
This data supports:
- Continuous review and improvement of safety and quality systems
- Education of our teams on safety and quality practices
- Transparent reporting on the care we provide
- Accountability across all levels of the organisation
We meet and aim to exceed all mandatory accreditation requirements.
Our approach is aligned to the National Safety and Quality Health Service (NSQHS) Standards, developed by the Australian Commission on Safety and Quality in Health Care in collaboration with governments, clinicians, and patients.
These standards provide a national framework to ensure care is safe and of a consistently high quality.
Your care, your rights
You are at the centre of your care.
We are committed to providing care that is safe, effective, and aligned to your needs. This includes:
- Involving you in decisions about your care
- Agreeing on care goals with you
- Seeking feedback from you and your carers
- Supporting you throughout your treatment
Learn more about your rights
Outlines how we work with patients, carers, and support people to ensure you are informed and involved in your care.
Australian Charter of Healthcare Rights
The Australian Charter of Healthcare Rights explains what you can expect when receiving healthcare in Australia.
It is available in multiple formats:
- English
- Languages other than English
- Aboriginal and Torres Strait Islander resources
- LGBTQIA+ resources
How we measure safety and quality
We collect and report clinical data to monitor the safety and effectiveness of the care we provide.
Safety and quality are measured as the number of incidents per 1,000 occasions of service. An occasion of service refers to any treatment or service provided to outpatients in a healthcare facility.
How we track performance
We report our safety and quality results quarterly across seven key areas of care.
Where available, we compare our results against national benchmarks to show how we are performing.
Fall rate: 0.11
Patient falls per 1,000 occasions of service (lower is better)
National Average: 2.0*
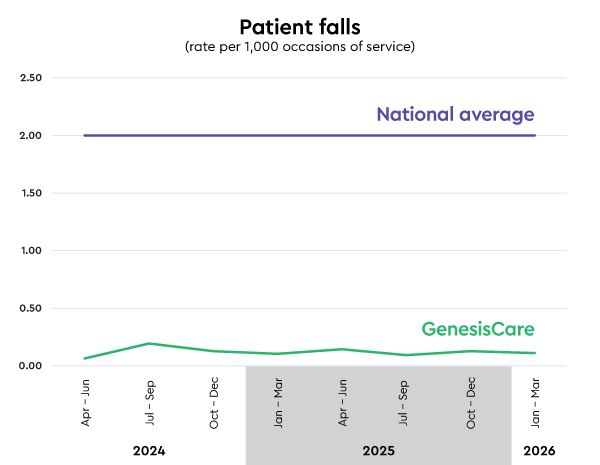
*AIHW 2021-22 Private hospitals admitted patient data for falls resulting in patient harm
Falls are one of the most common risks in healthcare, and preventing them is a priority.
We have processes in place to reduce the risk of falls, supported by staff education, incident reporting, and ongoing review to ensure these measures remain effective.
Things you can do:
You can help reduce your risk of falling by wearing well-fitting, non-slip shoes, bringing any walking or mobility aids to your appointment, and letting staff know if you have had a recent fall or feel unsteady on your feet.
Medication incident rate: 0.16
Incidents per 1,000 occasions of service (lower is better)
National Average: 1.0*
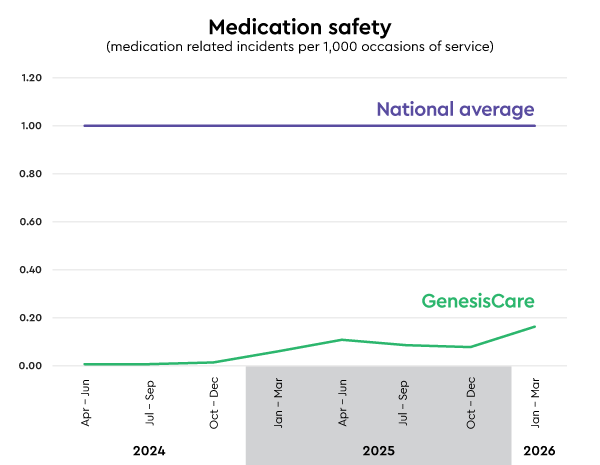
*AIHW 2021-22 Private hospitals admitted patient data for falls resulting in patient harm
Medication safety is a priority, and all incidents are taken seriously.
We investigate every incident to improve medication management and reduce the risk of future errors. We use a specialised oncology health information system to manage and document medications and treatment, supporting safe and accurate care.
Things you can do:
You can help by keeping an up-to-date list of your medications and being involved in your care. Let your treating team know about all medications you are taking, any allergies, and any changes since your last visit.
Clinical deterioration rate: 0.58
Patients experiencing a clinical deterioration during their care per 1,000 occasions of service (lower is better)
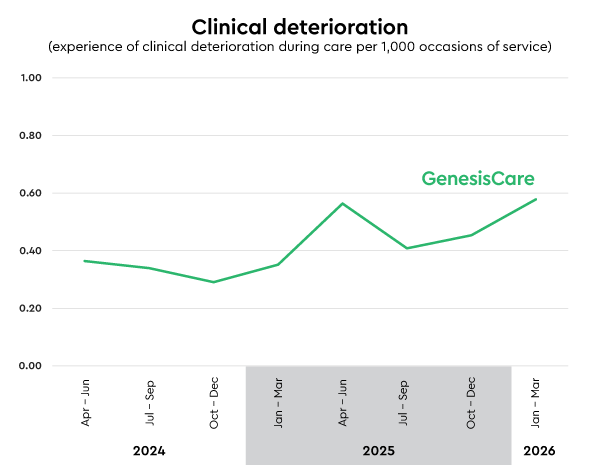
Recognising and responding to clinical deterioration is essential to patient safety.
We have systems in place to identify when a patient becomes unwell and respond quickly to prevent further deterioration. We also record and review transfers to hospital to ensure any learnings are used to improve future care.
Things you can do:
Let your treating team know if you feel unwell or notice any changes in your condition. This includes worsening symptoms or new symptoms. Early communication allows your care team to assess you promptly and make any necessary adjustments to keep you safe.
Patient identification rate: 0.04
Incidents per 1,000 occasions of service (lower is better)
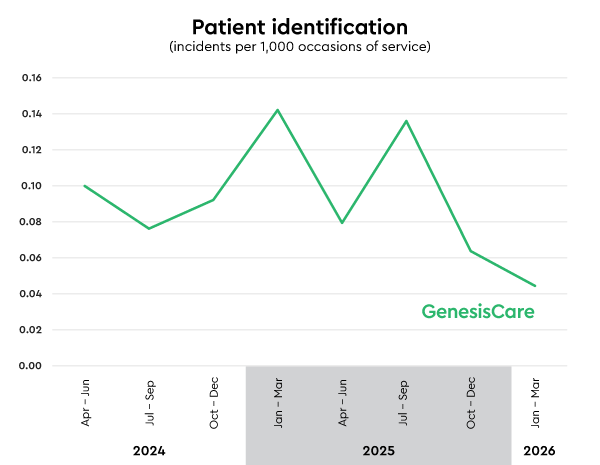
Correct patient identification is essential to delivering safe care.
We verify your identity at each stage of your care to ensure the right treatment is provided to the right patient. Our staff use three points of identification every time to prevent mix-ups and keep you safe.
Things you can do:
Answer identification questions when asked and check that your details are correct. Let staff know if you believe your identity has not been confirmed correctly before any treatment or procedure begins.
Healthcare associated infections
(HAI) rate: 0.01
Incidents per 1,000 occasions of service (lower is better)
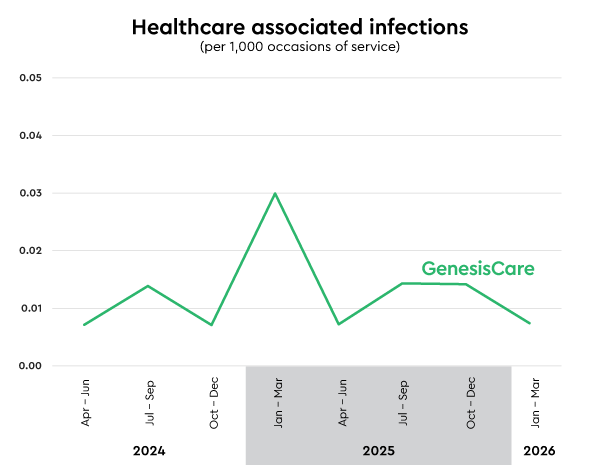
Good hand hygiene is one of the most effective ways to prevent infection.
Our program is aligned with the National Hand Hygiene Initiative (NHHI) and monitors compliance during patient care across all our sites.
Things you can do:
Wash your hands or use alcohol hand rub when entering and leaving the facility, and after any treatment or intervention. Let staff know before your visit if you have cold or flu symptoms. Family members, carers, or support people should not attend if they are unwell.
Pressure injuries and skin integrity incidents rate: 0.10
Incidents per 1,000 occasions of service (lower is better)
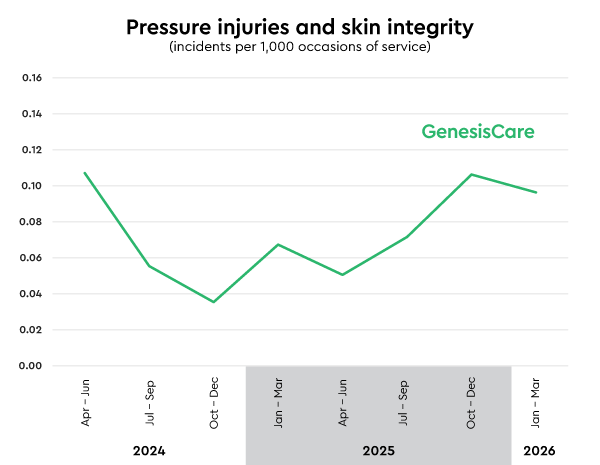
Maintaining skin integrity is an important part of your care.
We monitor and report on pressure injuries and other causes of skin breakdown, including changes that can occur during radiation therapy. Our clinical teams regularly assess your skin throughout treatment to help keep it healthy.
Things you can do:
Follow the skin care advice provided by your treating team and let them know if your skin becomes red, sore, or irritated.
Clinical handover error rate: 0.52
Errors or omissions per 1,000 occasions of service (lower is better)
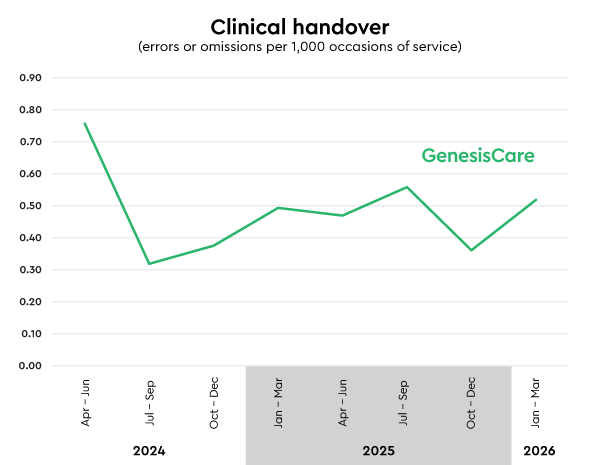
Clinical handover ensures your care is safely transferred between healthcare professionals.
This includes communication between referring hospitals, doctors, and GenesisCare staff. We use structured tools to support clear and consistent handover, and we keep you informed so you can contribute important information about your care.
Things you can do:
Stay informed and involved during your care. Ask questions and share any relevant updates about your condition, treatment, or medical history with your care team.

You are leaving our website
You are now leaving our website. GenesisCare do not control this content and therefore are not responsible for its accuracy or reliability.



